"Being uninsured is expensive"
A continuous struggle I’ve had since aging out of foster care is accessing and navigating healthcare services without health insurance. I know I am not alone in this; according to the Northwest Foster Care Alumni Study, more than half of young adults who have aged out of the system do not have health insurance and 61% do not have dental insurance. Though I am hopeful the new extension of the Affordable Care Act that allows former foster youth to receive health care benefits until age 26 will improve these figures, I still find them unacceptable. What makes this statistic so alarming is: “Youth in foster care face medical and mental health challenges at significantly higher rates than other children, often as a consequence of the circumstances that led to their removal from their home and sometimes exacerbated by their experiences in foster care” (Health Care of Youth Aging Out of Foster Care, American Academy of Pediatrics, 2012).
Being uninsured is expensive. I've paid close to $7,000 in emergency medical bills since coming to college and aging out of the system. My largest individual bill was over $4,000 and took me a year to pay off through monthly payment installments. This figure also does not include the recent $2,300+ bill I have sitting on my desk from an ER visit in March that I have yet to pay. Being uninsured costs me in other areas as well, such as my car insurance premium. My monthly payment is significantly higher due to my lack of health insurance.
I feel ashamed to admit that I am uninsured. Treating physical ailments and having access to health services feels as though it is one of the most basic human rights and needs. I have remedied my fear of disclosing my former foster care status by realizing nearly everyone encounters some form of family drama or life struggle. I cannot, however, remedy my feelings of shame, embarrassment, and frustration surrounding my lack of health insurance. It is an awful thing to rank and evaluate your self worth in the midst of great pain in the middle of the night. Far too many times have I said to myself, “How much money am I willing to pay for this pain to go away? What will be the risk if I do not seek professional help? Am I worth the trouble, or can I withstand the pain?” All of those healthcare taboos you’re warned about, such as not relying on the internet or WebMD to diagnose a problem, do not apply to the uninsured. WebMD was often my only option.
I whole-heartedly believe that my limited access to health care has caused further health concerns to develop. Consider my ankle, for example. I injured it in November of 2013. I decided to go to urgent care based on my friend’s recommendation, who is a nurse. I couldn’t put any weight on it and could hardly move it. After paying $200 cash just to be seen by the doctor, I had two sets of X-rays preformed (at an additional price) because they couldn't see through the swelling. I was told that that the doctor thought I had a hairline fracture but that I had to come back in a week after the swelling went down for another X-ray. I was given a prescription for pain medication that was too expensive for me to fill. I decided not to go back in for an additional X-ray due to fear of another large bill and borrowed a walking cast from an acquaintance instead. I thought my ankle was healed after a few months, despite the occasional shooting pain in my right foot, specifically near my toes. Lately, it's been getting a lot worse and I experience pain almost daily. I have thought about seeing a doctor but am waiting until I have health insurance in fear I will be referred to a specialist that will undoubtedly be expensive without insurance.
My ankle is only one thing on my list of health concerns I am eager to have addressed. Next on the list is having oral surgery to remove my wisdom teeth, which desperately need to be taken out. I am excited to report that – hopefully – I will officially have health insurance (including dental!) in 2 weeks from today. Learning this news felt almost as good as receiving my acceptance letter from grad school. After a 7-month application and re-application process through Medicaid, I have finally selected an approved plan and have already begun researching doctors in my area. To illustrate my difficult, lengthy application process, I’ve created this timeline:
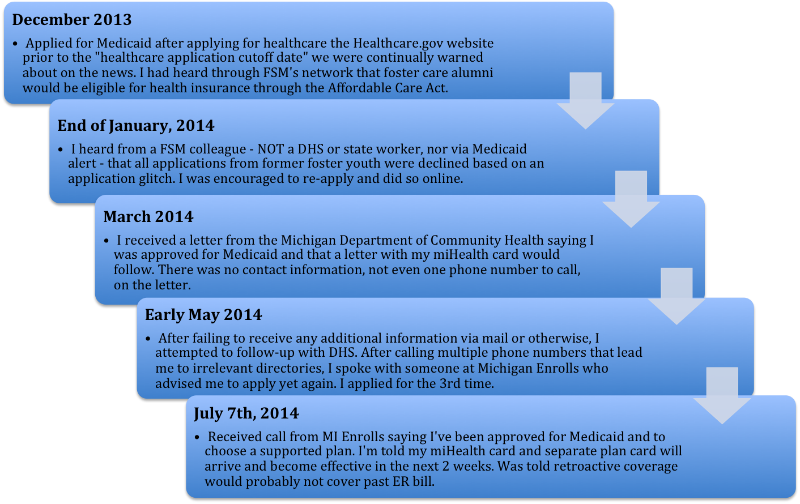
What was most difficult for me throughout this process was the division of services. When I finally did speak to someone at Michigan Enrolls and explained my situation to them, they kept advising me to “ask my worker.” I explained that, as an alumni of foster care, I did not have a DHS worker any longer. She then referred me to “my DHS caseworker” in charge of Medicaid, which again I did not have due to my unsuccessful enrollment. I was repeatedly told that the department I was speaking with couldn’t help me, and to try another division of services that I had already tried to contact. Whenever I would reference my time spent in foster care, the few people I spoke to had little to no knowledge of what this meant for me in terms of insurance options. On several occasions, I felt as though I was educating the Medicaid professionals on my insurance options, when it should be the other way around.
If you are a professional working with youth in or from foster care, I have a few recommendations to help students access healthcare:
- Make healthcare a priority. It is already one of Casey Family Programs’ Life Domains, but it must be treated with more urgency during conversations with students. “Adolescents often feel invulernable at [the transitionary] stage of development, so youth leaving foster care may need help understanding why their ongoing health care should be a priority” (Health Care of Youth Aging Out of Foster Care, American Academy of Pediatrics, 2012). Ask students when you first meet with them when their last doctor appointment was, if they are currently in any pain, or are struggling with any health concerns. If concerns arise, try to connect the student with appropriate resources and create a follow-up plan with them before they leave the office.
- I highly recommend that campus based support programs or other professionals working with young adults who have experienced foster care provide youth with some sort of guideline for healthcare expectations. After being in the system with such sporadic healthcare opportunities, I am not sure as an adult what is reasonable. How often should I see a dentist? What about a doctor? What are recommended tests and procedures for my age? Adding recommended timeframes for standard check-ups and medical tests to accessible resources in your organization or program would serve as a helpful reference for students.
- Help students read through insurance documents and ensure their understanding. Some of the terminology used can be confusing for students who aren’t accustomed to using it. I plan on making an “insurance cheat sheet” once I receive my plan information that easily spells out “Prescription Co-Pay: $10 per script, Office Visit Co-Pay: $10” or the like.
- Use your connections and utilize your network. If you have a colleague who works at the DHS office, see if you can get them in touch with the student in need. If the student you’re working with is having difficulty accessing the system or understanding their options, ask your professional peers if other students are encountering the same problems.
- If there is a deadline, help the student keep it. My campus coach was awesome at reminding me of important scholarship or service-related deadlines. She would add it to her calendar and send me text message reminders or even calendar event invitations via e-mail that would automatically remind me when the due date was approaching. Student life can feel extremely busy and overwhelming, and every little friendly reminder helps.
- The single most important thing a professional, agency, or organization can do when increasing health care (and other positive) outcomes for young people from foster care is to ensure their resources are easy to access and comfortable for students and professionals to navigate. After Genanne and Maddy at Fostering Success Michigan (FSM) first read through this blog, they realized that the numerous resources available on the FSM website might be difficult for partners to find and sift through in search of answers to student healthcare dilemmas. Immediately after this realization, they decided to create a compiled resource for both students and professionals. This toolkit is easy to read and provides immediate answers as well as direction to relevant resources. What was so meaningful to me as a student is that FSM listened to my needs and did what they could to improve their work. Instead of adopting the attitude that we as students and consumers of services need to adapt to the way information is presented, FSM improved the presentation of their information to be easier for students to access. Genanne was extremely interactive throughout the experience and asked me to look over her drafts, appreciating my input and suggestions. All of the guides at FSM are created with (and sometimes exclusively by!) students, which is imperative for organizations that serve the young adult population. When Genanne told me over the phone that reading about my dilemma sparked her to seek change and make improvements, I felt empowered. I felt validated for voicing my experience and excited that my concerns with the current system in place could actually bring about systematic change.
The Guide to Accessing Healthcare can be found here: http://fosteringsuccessmichigan.com/library/how-to-get-health-care
If you have any questions, or receive any messages that say that you have been denied coverage, There is help available! Please contact:
Leslie Adams, Foster Care Health Analyst
Child Welfare Medical Unit
Office of Child Welfare Policy and Programs
Michigan Department of Human Services,
235 S. Grand Avenue, Suite 514,
P.O. Box 30037, Lansing, MI 48909
Phone: 517-335-0988
Fax: 517-335-7789
AdamsL4@michigan.gov